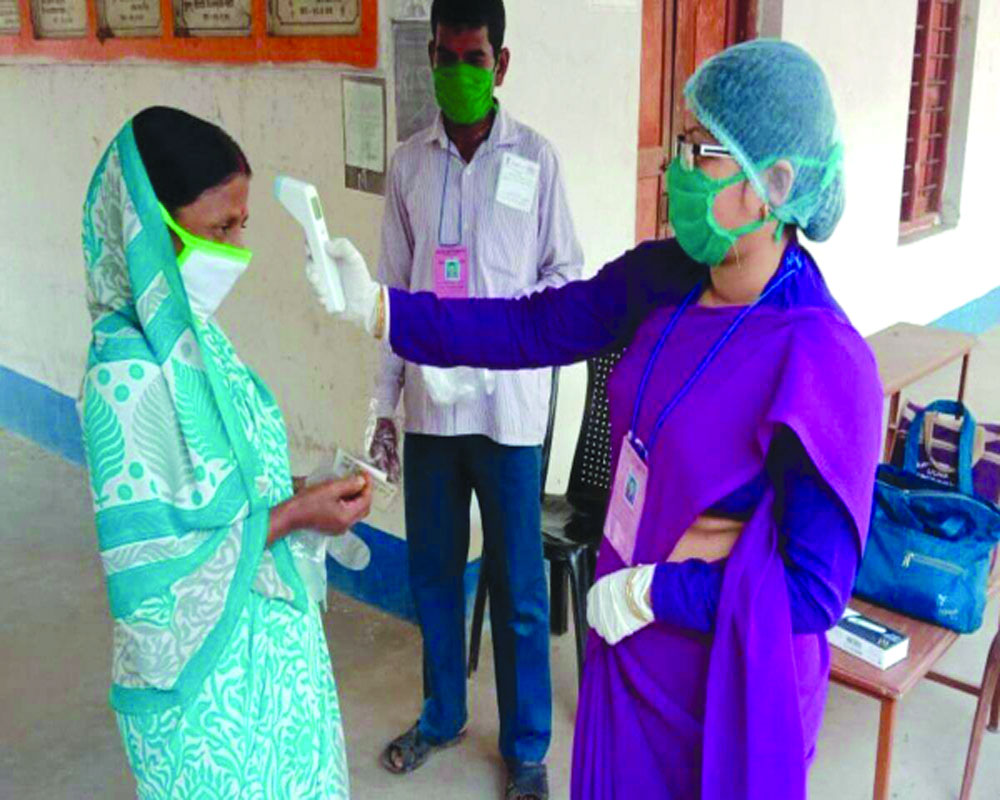
Villagers in remote areas of the country stared at a healthcare disaster during the pandemic, says Rajesh Nirmal
Around 65.5 per cent of India’s total population resides in rural areas. Tucked away in some of the remotest corners of the country, these areas are often characterised by poor development infrastructure. Unavailability of and inaccessibility to health-care services is the most crucial gap. In terms of accessing health-care benefits, there are certain barriers faced by the rural population, especially women. In current Covid times, these barriers have multiplied, making the lives of the rural populations even more challenging.
During the different phases of lockdown, people who can access smartphones, the internet, and correct information, could reach out to doctors for online consultation. On the other hand, more than half of the rural population continued to rely upon the medicines they identify only by their colour, mostly available at the local medical stores. “Almost everyone in our village depends on these locally available medicines. We have a habit of curing sickness without visiting any doctor. As the nearest government hospital is eight to 10 km away from our village, no one has time and other resources to be spent on hospital visits,” shared 34-year-old Laalti Devi from Rampur Babuan village, Sultanpur district in Uttar Pradesh.
Laalti, whose husband migrates to the city in search of work, informed that in his absence, she looks after the family. “In such a scenario, if anyone from my house gets sick, we get medicine from the medical store and follow the instructions given by the pharmacist,” she said. Visiting private hospitals is not an option for the rural poor who find it difficult to make ends meet.
During both the first and second wave, the majority of district hospitals were converted to Covid facilities, further limiting the access of villagers in case of emergencies. According to Laalti, during the horrific waves of the pandemic, people feared even thinking about visiting the hospitals. They are still afraid that they will get infected with Covid if they will visit hospitals. They are also frightened that they may be forced to get vaccinated if they will visit the government health-care facilities.
Sharing her experience regarding obtaining medical treatment during the pandemic, Laalti informed, “Last year, I had developed certain health complications. With my husband not around, I had no one to seek advice from. The fear of Covid was such that I decided to wait. After the lockdown was lifted and my husband managed to return, we went to the hospital for treatment. The infection, however, had spread because of the delay in treatment.”
47-year-old Prabha Devi, another local resident of the village, had to undergo uterus removal surgery. As the hospitals were full of Covid patients, she could not utilise the services of government hospitals. “I wanted my aunt to undergo surgery in the district hospital, but I was not capable of that kind of hustle. Due to Covid, people with other health complications were not being treated properly. Doctors were overwhelmed with the Covid cases,” shared Sandeep, a relative of Prabha Devi.
“Taking all the factors into consideration, my family had decided that even if they had to take a loan or sell our fields, my treatment will be done at a private hospital because they could not put my life at stake,” rued Prabha Devi.
Not every woman is lucky to have access to financial resources to get their illness treated. They keep suffering in silence. One of the reasons that prevent rural women from receiving institutionalised health-care is the unavailability of hospitals in their villages. This year, the Finance Minister has, however, allocated ` 64,185 crores towards strengthening health services in rural India. Besides, ` 35,000 crores have been set aside to tackle the pandemic, which is planned to be spent on primary, secondary, and tertiary health-care. Overall, there has been a 137 per cent increase in the national budget as compared to last year. It is, however, not only the infrastructure that needs to be strengthened.
The issue of health-literacy among the rural populations, especially women, also needs to be addressed as it impacts their ability to apprehend health information provided by frontline workers like ASHA. Due to poor health literacy, women feel reluctant to seek healthcare as they fear communicating with healthcare providers. Additionally, low health literacy impacts the implementation of government initiatives.
Drawing upon the experiences of the villagers, especially women, it is quite clear that a strong health-care network must be established in rural areas. Using the budget allocated by the union government, the local administration should devise a special program where the doctors and medicines should be accessible to villagers, and a strong healthcare work-force should help address the health illiteracy gap in these rural areas.
—Charkha Features